Breathing for tomorrow a mother, a doctor, and Kenya’s war against Pneumonia
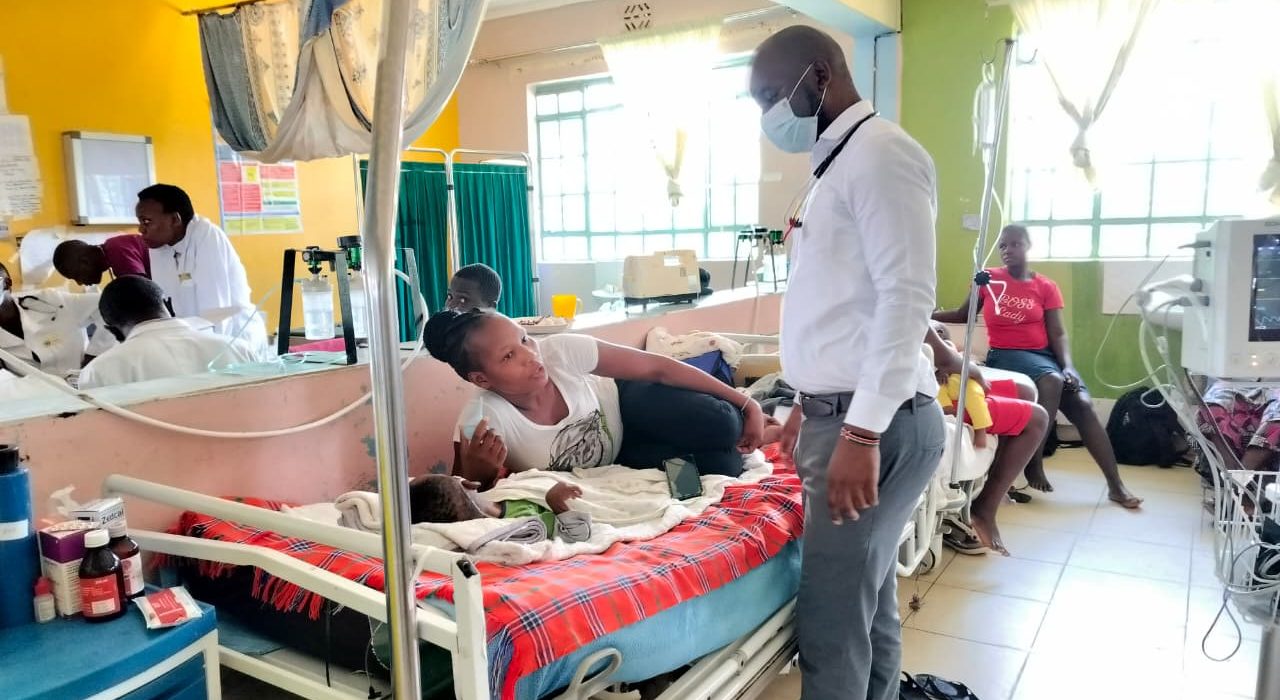
The air in the paediatric ward is thick with disinfectant and worry. A half-light spills through yellow curtains, softening the edges of metal beds lined shoulder to shoulder.
Oxygen machines hiss like sleeping animals. Mothers sit upright in plastic chairs, eyes fixed on their children’s faces, counting breaths.
At the third bed from the door, Millicent Wanyonyi cradles her eight-month-old son, Brian. His chest trembles with every inhalation; a clear tube taped to his tiny nostrils snakes toward the humming cylinder at his bedside.
Wrapped in a red-and-blue Maasai shuka, he looks far too small for the hospital mattress. Beside him, a bottle of cough syrup, a folded feeding cloth and a phone sit untouched.
“I lost my firstborn daughter to pneumonia,” Millicent says, her voice scarcely a whisper. “When Brian started coughing, I prayed it wasn’t the same thing.
But here we are again.” For four nights she has slept in snatches, curled on the edge of the bed. Her husband, a boda-boda rider, sold their only goat to pay for medicine.
“Sometimes I think God is testing me twice,” she says. “But I’m not ready to bury another child.”

Across the room, Dr Dickens Lubanga strides from bed to bed, a stethoscope swinging against a crisp white shirt. The fabric creases at the elbows from long hours; a surgical mask hides the fatigue in his face but not the urgency in his eyes.
“How’s he this morning?” he asks, kneeling beside Millicent. “He coughed all night,” she murmurs.
Lubanga listens to Brian’s chest, adjusts the oxygen flow, and offers a small nod. “His lungs are weak, but he’s fighting,” he says.
“Don’t give up.” The ward hums like a living organism: nurses in white coats record temperatures, the soft clink of IV stands echoes down the corridor, and somewhere a mother hums a lullaby off-key. “Every week we admit thirty to forty children with pneumonia,” Lubanga says.
“Three-quarters come from Bungoma, Mt Elgon and Mumias places where poverty, cold air and smoke rule the nights. Pneumonia thrives where life is hardest.”
Worldwide, the disease kills nearly 700 000 children under five years every year, one every twenty seconds, according to the World Health Organization (WHO). In Kenya, it claims between 8,000 and 10,000 young lives annually, just behind malaria.
For decades, malaria defined the western region’s tragedy; now another invisible killer has taken its place. “It’s not just infection,” Lubanga explains.
“It’s poverty, malnutrition, and late treatment.” Seven in 10 households around Lake Victoria still cook with firewood or charcoal, Kenya’s 2023 Demographic and Health Survey reports.
The smoke clings to mud-walled homes, infiltrating infant lungs still learning how to breathe. “By five years, some damage can’t be undone,” the doctor says.
Between May and August, pneumonia cases jump 40 percent as cold, wet weather settles over the hills a season sharpened by climate change. “Cold constricts lungs,” Lubanga says. “But poverty kills faster no warm clothes, no heating, no food.”
For Millicent, hunger is routine. “We eat once a day roasted maize or porridge,” she says. “I thought it was hunger making him weak.”
Treating mild pneumonia in a public hospital costs KSh10,000 to KSh15,000; private wards charge KSh50,000 or more, and a severe ICU case can drain half a million.
“Parents delay because they can’t pay,” Lubanga says. “By the time they arrive, the child is gasping.” Each week at the hospital means lost income, missed harvests, deepening debt. “A sick child doesn’t just break hearts,” the doctor adds. “It breaks livelihoods.”

In 2023, Bungoma installed a solar-powered oxygen plant that now feeds the paediatric annex. Neonatal deaths dropped by nearly a third, yet shortages and fatigue persist. “Parents self-medicate,” Lubanga sighs.
“They buy antibiotics without prescriptions. It’s building resistance the next silent pandemic.”
Kenya introduced the pneumococcal conjugate vaccine in 2011.
Today more than 90 percent of children are protected, and in Bungoma, Vihiga and Nandi counties coverage touches 100 percent. Still, inequality persists. “The public vaccine shields a child for about a year,” Lubanga says.
“The stronger version lasts five years but costs KSh7,500 to KSh8,000 per dose. Only the rich can afford it.” He believes state bulk purchase could cut the price to KSH2,000. “That policy could save thousands.”
At two in the morning the ward trembles under rain on the iron roof. The oxygen monitor beside Brian shrills; his level falls to 88 percent.
Lubanga races over, adjusts the mask, presses a stethoscope to the tiny chest. “Come on, Brian,” he whispers. Millicent grips her rosary. The numbers climb 90 … 94 … 97. The alarm quiets.
“He’s stable,” the doctor says. Millicent exhales a sob of relief. “Maybe God still remembers us.”
Across sub-Saharan Africa, seven of the world’s ten worst-hit countries are on this continent, and pneumonia kills more than 350,000 African children each year.
Four in five of those deaths could be prevented with vaccines, breastfeeding, clean air and oxygen. UNICEF’s 2025 Global Action Plan for Pneumonia and Diarrhoea says that reaching every child could save 4.2 million lives by 2030.
“The science exists,” a UNICEF Kenya officer says. “The tragedy is inequality.”
Kenya’s Ministry of Health vows to equip all 47 counties with oxygen plants by 2026 and to weave pneumonia control into Universal Health Coverage. Digital tracking through DHIS2, solar cold-chain storage and community health volunteers are closing old gaps.
Every Breath Counts; Every Action Matters rings through rural clinics as a promise.
By dawn, the ward softens into pale light. Brian stirs, his breathing slow but sure. The nurse unclips the oxygen line. Millicent leans close, her eyes glistening.
“He’s breathing by himself,” she says. “Maybe this time, I get to take him home.” Outside, Bungoma wakes under a silver mist.
Women balance bundles of firewood on their heads. A rooster crows somewhere beyond the hospital gate. Each mother who leaves the annex carrying a living child is one less statistic, one more victory against an ancient enemy.
By 2025, health data show that Bungoma and Vihiga counties lose about a thousand under-five children to pneumonia each year, while Kenya’s national toll hovers around 10,000.
During the cold season, admissions rise 40 percent. Sixty-two percent of local health facilities now have functional oxygen compared with 45 percent across Africa and more than 90 percent globally.
Vaccination coverage in western Kenya averages 97 to 100 percent, higher than the 90 percent national mean and the 60 percent continental average. Treating a single case can cost anywhere between 10 000 and 500 000 shillings, a reminder that survival is often a question of money as much as medicine.
In Bungoma’s crowded pediatric annex, those numbers have faces. They are Brian’s shallow breaths, Millicent’s trembling hands, and Dr Lubanga’s weary eyes. They are the sounds of oxygen, faith, and resilience.
And as the machines hum on, the story of every child who leaves this ward alive whispers the same truth to the world every breath is a right, not a privilege.










